January 20, 2016 — Patients enrolled in high-deductible health insurance plans have lower rates of use and lower costs for imaging tests, suggests a study in the February issue of Medical Care.
"Increased patient cost-sharing may contribute to reductions in diagnostic imaging utilization and spending," reported Sarah Zheng, MA, of Boston University Questrom School of Business and colleagues. But they cite potential concerns over whether high-deductible plans may discourage use of medically recommended, "high-value" imaging studies as well as less critical, "low-value" tests such as lumbar spine magnetic resonance imaging (MRI) for lower back pain.
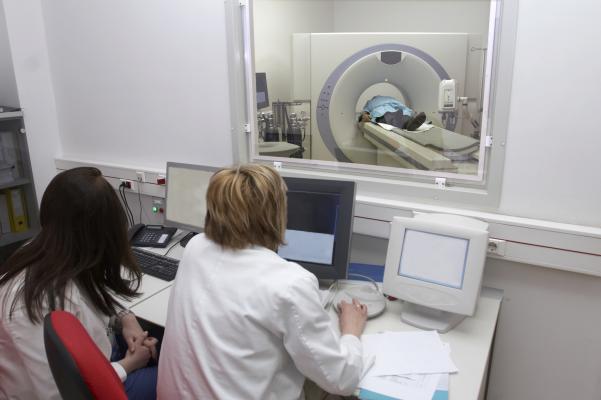
Using an insurance database including more than 21 million adults, the researchers compared use rates and costs of imaging studies—X-rays, computed tomography (CT) or MRI scans and others—for patients with and without high-deductible insurance plans. More Americans are enrolling in high-deductible insurance plans, which have relatively low premiums but higher out-of-pocket costs.
Insurance plans with an annual deductible of at least $1,200 for individuals and $2,400 for families were considered high-deductible. Such plans increase the patient’s share of the cost of healthcare services, which proponents of high-deductible plans argue helps reduce overuse.
In the 2010 insurance data used, about 8 percent of patients were covered by high-deductible plans. After controlling for age, sex, geographic location and health status, individuals enrolled in high-deductible plans used 7.5 percent fewer imaging studies than those in other plans. "This difference in imaging utilization corresponded to a 10.2 percent difference in imaging payments," the researchers wrote.
Patients in high-deductible plans were less likely to undergo any diagnostic imaging study—a difference of 1.8 percentage points. However, once an enrollee had at least one imaging test, being in a high-deductible plan had little effect on the total use of and payments for imaging studies.
When patients were categorized by health status, the effects of high-deductible plans on use rates and costs of imaging studies were largest in the least-sick group, the group that was unlikely to reach the deductible without imaging use.
Previous research has shown that high-deductible insurance plans lead to reduced use of a wide range of healthcare services: hospital care, office and emergency department visits, and others. The new study is the first to directly address the effects on use of diagnostic imaging studies nationwide. "As diagnostic imaging can have important downstream care and cost implications, having the right level of high-value utilization is an important policy priority," the researchers wrote.
The results show that high-deductible plans are associated with lower use of imaging studies. That's an important finding, given the high cost of imaging tests in the U.S. healthcare system. From 2000 to 2014, Medicare spending for imaging almost tripled, from $3.6 billion to $10 billion.
However, the study was unable to determine whether the reduced imaging use associated with high-deductible insurance was high- or low-value—an important consideration for patient outcomes. Along with previous studies, the results raise concerns that "high-deductible health plans may be a blunt instrument reducing all diagnostic imaging, rather than helping physicians and patients choose high-value imaging," the researchers wrote.
Zheng and coauthors emphasize the need for further studies to understand the care and cost implications of high-deductible plans. They conclude, "Better patient awareness and education may be a crucial part of any reductions in diagnostic imaging utilization."
For more information: www.journals.lww.com

 August 06, 2024
August 06, 2024