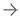
Image courtesy of Zeiss
December 21, 2020 — According to recent studies, an increase in the COVID-19 positivity rate correlates to an increase in mortality from non-coronavirus-related diseases. This includes breast cancer, and researchers believe fear of contracting the virus compels patients to stay home instead of completing their post-lumpectomy radiotherapy regimens.
However, physicians at Mercy Medical Center are countering this trend with a procedure called Targeted Intraoperative Radiotherapy, or TARGIT-IORT using the Intrabeam System from ZEISS. Mercy was the first hospital in Maryland to acquire the INTRABEAM Radiotherapy System in 2012, and remains the only hospital in the state to offer patients the INTRABEAM system.
IORT is a single treatment which takes the place of external beam radiation therapy (EBRT) done at the time of the lumpectomy.
“Unlike external beam radiation therapy (EBRT) which requires up to 30 visits to the radiotherapist, TARGIT-IORT achieves the same clinical outcomes with one dose of targeted radiation delivered from inside the breast during surgery immediately following the removal of the tumor,” explained Neil B. Friedman, M.D., FACS, Director of The Hoffberger Breast Center at Mercy.
Not only does TARGIT-IORT mitigate the side effects normally associated with irradiating the entire breast multiple times, it may lessen or even eliminate unsafe additional outside trips during the pandemic.
“With IORT, patients experience less irritation of healthy breast tissue, minimized exposure to the chest cavity and underlying organs, and fewer skin reactions, such as redness, rashes, and irritation. And now, given COVID-19, risk to the patient is reduced by eliminating the need to make multiple visits to the hospital for radiation treatments,” said Maria C.E. Jacobs, M.D., Director of Radiation Oncology at Mercy.
Since March of 2020, overall deaths in the United States have increased 20% compared to predicted mortality rates, according to a study published last month in the Journal of the American Medical Association. Yet fully one third of these “excess deaths” are due to causes other than COVID-19, leading researchers to conclude that the coronavirus is impacting Americans’ decisions to seek medical care for other diseases, including cancer. The study found a direct correlation between COVID-19 surges in the spring and an increase in non-coronavirus-related deaths during the same period of time.
“One of the trends the researchers noted is that treatment compliance – for a variety of diseases – seemed to be disrupted at a rate proportional to the severity of the pandemic,” Friedman said. “If elevated coronavirus levels earlier this year caused patients to abandon their radiotherapy regimens, we have every reason to expect compliance challenges to drastically increase again during the anticipated ‘second wave’ this fall and winter.”
Two additional studies have demonstrated the importance for patients to adhere to their cancer treatment regimen while also taking precautions to minimize their exposure to both radiation and potential coronavirus infection. A study published last month in the American Cancer Society journal Cancer found an increase in fatal outcomes among patients hospitalized with COVID-19 who had also recently undergone traditional post-surgical radiation therapy. Unfortunately, a second study found that delaying or skipping radiotherapy is also not a viable option. Published this month in the BMJ, researchers saw a significant increase in mortality among patients who deferred breast cancer treatment by as little as four weeks.3 Single-dose TARGIT-IORT, however, may decrease or eliminate both of these issues.
EBRT vs. TARGIT-IORT
External beam radiation therapy (EBRT) involves treating the entire breast from the outside. Although the radiation therapy is directed to the breast rather than the surrounding tissues, the proximity of the heart, lungs and skin limit the dose of radiation that can be given at any one time. This leads to a prolonged treatment course of 3-6 weeks following surgery. The TARGIT-IORT treatment administers the radiation dose from inside the breast at the time of surgery, precisely where it is needed. This allows the radiation oncologist to deliver a much higher dose at one time, avoiding irradiation of vital adjacent organs such as the lungs and heart.
TARGIT-A TRIAL
The effectiveness of TARGIT was investigated in an international study called the TARGIT-A Trial, a clinical trial that compared partial breast single dose targeted intraoperative radiotherapy (TARGIT-IORT) to 3 to 6 weeks of post-operative whole breast radiotherapy among women undergoing lumpectomy for early stage invasive ductal breast cancer. The clinical trial demonstrated equal breast cancer recurrence rates and equal cancer survival rates among recipients of targeted IORT during lumpectomy compared to those receiving multiple weeks of whole breast radiation after lumpectomy. The paper was published August 19 in BMJ4.
With long term follow-up (median 8.6 years, maximum 18.9 years), the TARGIT-A Trial demonstrated no significant difference in the 5- year local recurrence rates and 8.6 year local recurrence-free survival rate, breast cancer survival rate, and overall survival rate. Women receiving targeted IORT had a significantly lower risk of dying from other causes (e.g., heart disease or other cancers).
For more information: http://www.targetbreastcancer.org

 April 24, 2025
April 24, 2025