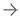Carsten Schroeder, M.D., thoracic surgical oncologist at the Georgia Cancer Center and Medical College of Georgia at Augusta University in the hybrid OR. Image courtesy of Phil Jones, Senior Photographer, Augusta University
September 26, 2018 — When it comes to surviving cancer, early detection and treatment could be the key to a patient's survival. Thanks to an investment by Augusta University Health in a hybrid operating room, a surgeon can now diagnose and treat patients with lung cancer faster than is possible in a traditional operating room.
Representing a paradigm shift in thoracic surgery, the hybrid operating room combines multiple techniques into a single appointment, eliminating multiple clinical visits for improved patient experience and outcomes.
"Before I started using the hybrid operating room, it could take up to six weeks just to get a diagnosis," said Carsten Schroeder, M.D., thoracic surgical oncologist at the Georgia Cancer Center and Medical College of Georgia at Augusta University. "Having the hybrid OR and all of its technologies at Augusta University Health allows me to tailor the patient's care plan in one day instead of having to schedule multiple follow-up appointments."
Working with Philips through a long-term partnership model that allows for co-creating of clinical solutions, Augusta University Health opened its hybrid operating room in May 2017. It brings multiple techniques into a single space:
- Navigational bronchoscopy, allowing Schroeder to locate tumors in a person's lungs;
- Percutaneous biopsy, which gives Schroeder the ability to biopsy a small section of a lesion to see if it's cancerous;
- Fiducial marker placement to mark the tumor to make sure the entire mass is removed; and
- Video-assisted thoracoscopic surgery, allowing him to use a tiny video camera to operate inside a person's chest cavity.
In the hybrid OR, all of these techniques are assisted by intra-operative cone beam computed tomography (CT) imaging, which captures images of the inside of a person's chest and allows Schroeder to see the tumor and form the best surgical strategy to biopsy or remove it safely.
"The reasoning behind using the hybrid OR is to present a more efficient workup and treatment process to ultimately benefit patient survival," Schroeder said. "We can do that by shortening time from diagnosis to treatment while increasing cost-effectiveness and optimizing utilization."
According to research from the American Cancer Society (ACS), one in four cancer deaths can be attributed to lung cancer. This makes it the No. 1 cause of cancer deaths in men and women. The ACS said lung cancer kills more people each year than breast cancer, prostate cancer and colon cancer combined. One reason why the statistics are so grim, Schroeder said, is that it can be harder to detect and diagnose smaller tumors in the lungs. This means by the time they can be found and treated, they are at a more advanced stage.
Since moving his team into the hybrid OR 15 months ago, Schroeder has been collecting data on the outcomes of his patients. The data compiled included 25 patients. His findings, which he said show a paradigm shift in patient care, were published in Innovations: Technology and Techniques in Cardiothoracic and Vascular Surgery in August 2018.
"Additionally, we reviewed the medical charts of 11 patients," he said. "Each of those patients underwent a same-day bronchoscopy, CT-guided biopsy and surgical resection, if indicated, in the hybrid OR."
Of those 11 patients, 10 had a successful diagnosis in one setting. Six of those 11 were diagnosed with the cone beam CT-guided biopsy. Four of those six patients went on to have a surgical resection of their lung to have the nodule removed.
"Not only does the hybrid OR allow us to decrease the time between diagnosis and treatment, it also allows us to detect smaller tumors in a person's lungs," Schroeder said. "Before, we would have to wait for the tumor to grow larger or increase in density."
For more information: www.journals.lww.com/innovjournal
Reference


 September 12, 2024
September 12, 2024